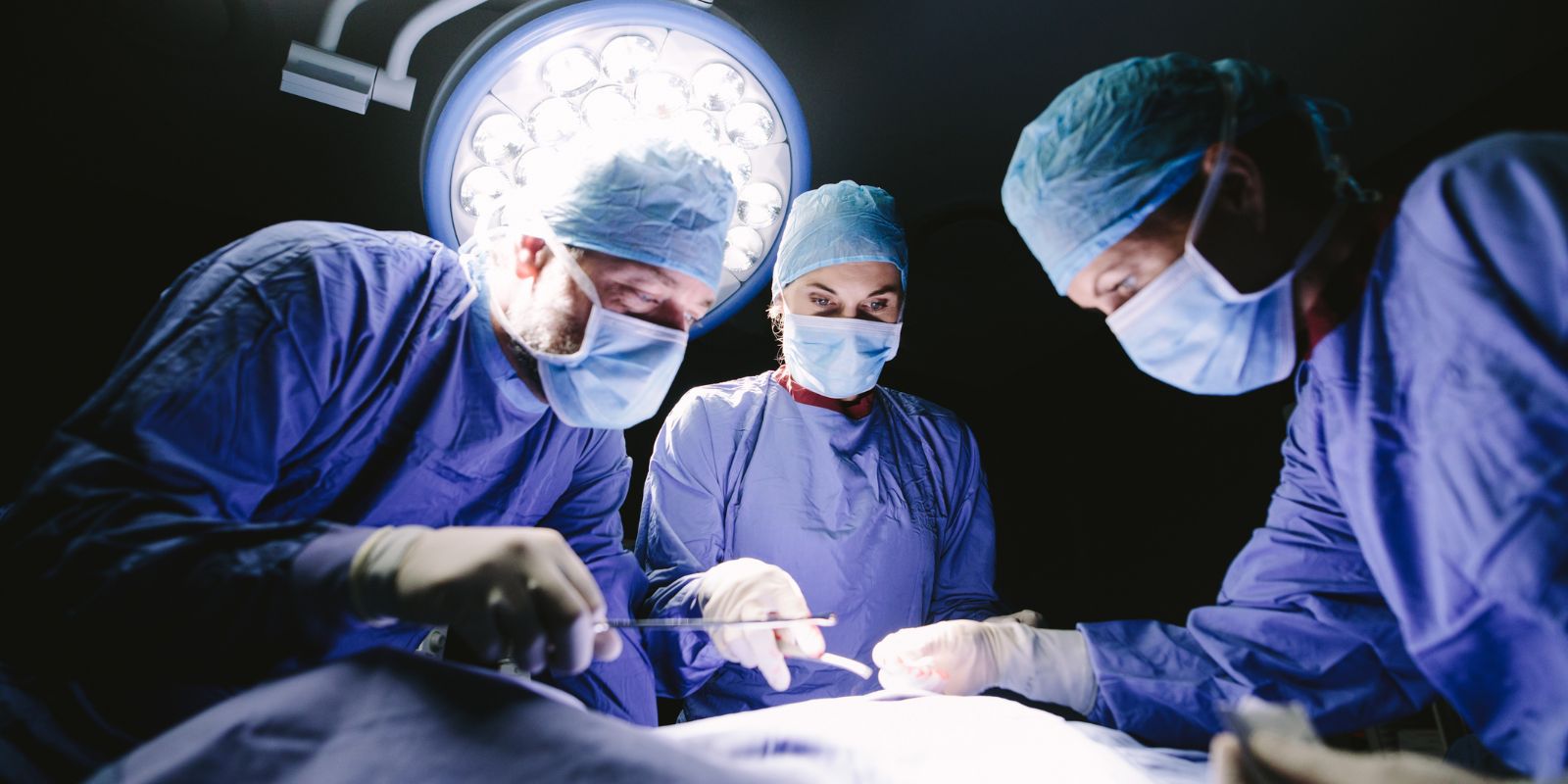
In today’s fast-evolving healthcare landscape, hospital staffing is no longer just about filling vacancies. It is about building a resilient, agile, and performance-driven workforce that ensures operational excellence while delivering safe, high-quality patient care. From emergency departments to intensive care units, the right staffing strategy directly impacts clinical outcomes, patient satisfaction, regulatory compliance, and financial performance.
Hospital administrators worldwide, including leading institutions like Mayo Clinic and Cleveland Clinic, emphasize workforce optimization as a central pillar of operational success. These institutions demonstrate how structured staffing models, strong leadership, and data-driven planning can transform hospital performance.
This article explores how hospitals can implement effective staffing strategies to achieve operational excellence.
1. Understanding Operational Excellence in Hospitals
Operational excellence in healthcare refers to the consistent delivery of high-quality patient care with maximum efficiency and minimal waste. It integrates clinical efficiency, administrative coordination, cost control, compliance adherence, and patient-centric service.
Staffing plays a critical role in achieving these goals. When hospitals are understaffed, patient wait times increase, staff burnout rises, and medical errors become more likely. Conversely, overstaffing inflates operational costs and reduces productivity. Therefore, achieving balance is essential.
2. Strategic Workforce Planning
Strategic workforce planning involves forecasting staffing needs based on patient volume, case complexity, seasonal trends, and service expansion plans.
Key elements include:
- Patient census forecasting
- Skill mix planning
- Shift optimization
- Succession planning
- Emergency surge capacity
Hospitals must analyze historical data to predict future demand. For example, flu season or regional outbreaks can increase admissions dramatically. Without proactive workforce planning, service quality suffers.
Advanced hospitals use predictive analytics tools to optimize staffing levels in real time. This reduces overtime expenses and prevents workforce fatigue.
3. Right Skill Mix and Competency Alignment
Operational excellence is not achieved by numbers alone—it requires the right combination of skills.
A balanced staffing model includes:
- Registered nurses
- Nurse practitioners
- Physicians
- Allied health professionals
- Technicians
- Administrative staff
Each department requires specialized competencies. For example:
- ICU requires critical care-certified nurses
- Emergency units require trauma-trained staff
- Surgical units require operating room specialists
Hospitals must align staffing structures with service complexity. Cross-training programs also enhance flexibility, enabling staff to support multiple departments during peak demand.
4. Reducing Burnout and Enhancing Retention
Staff burnout is one of the biggest threats to hospital operational excellence. High stress, long shifts, and emotional fatigue lead to turnover and reduced productivity.
Strategies to improve retention include:
- Flexible scheduling
- Mental health support programs
- Fair workload distribution
- Performance recognition systems
- Continuous professional development
Globally recognized institutions such as Johns Hopkins Hospital invest heavily in staff well-being programs, understanding that employee satisfaction directly influences patient care quality.
When hospitals prioritize workforce engagement, they see measurable improvements in efficiency and service consistency.
5. Leveraging Technology for Workforce Optimization
Technology plays a transformative role in hospital staffing.
Key digital solutions include:
- Automated scheduling software
- Workforce analytics dashboards
- Attendance and shift tracking systems
- Telemedicine integration
Hospitals using workforce management systems can quickly adjust staff deployment based on real-time patient admissions. Technology minimizes manual scheduling errors and enhances transparency.
Telehealth has also changed staffing dynamics. Physicians and specialists can now provide consultations remotely, optimizing resource utilization and reducing onsite staffing pressure.
6. Flexible Staffing Models
Modern hospitals increasingly adopt flexible staffing structures, including:
- Per diem staff
- Float pools
- Contract-based professionals
- Temporary surge teams
These models allow hospitals to adapt quickly during peak periods without permanently increasing fixed labor costs.
For example, during global health crises such as the COVID-19 pandemic, hospitals worldwide relied on flexible staffing systems to manage sudden patient surges.
A blended workforce approach ensures operational continuity without excessive financial strain.
7. Data-Driven Decision Making
Operational excellence demands measurable performance indicators.
Important staffing metrics include:
- Nurse-to-patient ratio
- Overtime hours
- Staff turnover rate
- Patient wait time
- Readmission rate
- Bed occupancy rate
Hospitals should regularly review these KPIs to identify inefficiencies. Data transparency enables leadership teams to make informed decisions and continuously refine staffing strategies.
Benchmarking against industry leaders helps identify gaps and improvement opportunities.
8. Compliance and Accreditation Standards
Healthcare staffing must align with regulatory and accreditation requirements. Compliance ensures patient safety and institutional credibility.
Organizations like The Joint Commission establish staffing guidelines that influence hospital operational standards.
Failure to comply can lead to:
- Legal penalties
- Financial losses
- Reputational damage
- Patient dissatisfaction
Therefore, staffing policies must incorporate credential verification, training documentation, and regulatory alignment.
9. Training and Continuous Development
Operational excellence requires a learning culture.
Hospitals should invest in:
- Clinical training programs
- Leadership development
- Simulation-based education
- Digital skills training
Continuous learning improves competency, reduces errors, and enhances teamwork.
Training also supports career growth, which increases retention and workforce stability.
10. Leadership and Communication
Strong leadership is essential for operational excellence.
Hospital leaders must:
- Maintain open communication
- Provide clear performance expectations
- Encourage feedback
- Resolve conflicts effectively
Transparent communication builds trust across departments and strengthens collaboration between clinical and administrative teams.
Leadership development programs prepare mid-level managers to handle workforce challenges efficiently.
11. Financial Efficiency Through Smart Staffing
Labor costs often account for 50–60% of hospital operating expenses. Therefore, staffing optimization directly impacts financial performance.
Cost-effective strategies include:
- Minimizing overtime
- Reducing agency dependency
- Improving productivity per shift
- Streamlining workflows
Balanced staffing reduces waste without compromising care quality.
Financial sustainability supports long-term operational excellence.
12. Building a Patient-Centric Workforce
Operational excellence ultimately revolves around patient satisfaction.
A patient-focused staffing model ensures:
- Reduced wait times
- Faster diagnosis
- Better communication
- Higher care coordination
When staff are adequately trained and not overburdened, they can provide compassionate, attentive care.
Positive patient experiences enhance hospital reputation and long-term growth.
Conclusion
Hospital staffing is the backbone of operational excellence. It influences clinical outcomes, financial performance, employee engagement, and patient satisfaction. By adopting strategic workforce planning, leveraging technology, investing in training, and maintaining compliance standards, hospitals can create a resilient and high-performing workforce.
Institutions that treat staffing as a strategic priority—not just an HR function—consistently outperform competitors. A data-driven, flexible, and employee-centered staffing approach ensures operational efficiency while maintaining the highest standards of patient care.
In an increasingly complex healthcare environment, hospitals that optimize staffing today will lead the healthcare ecosystem tomorrow.